Can Receding Gums Grow Back? What Your Kansas City Dentist Wants You to Know
It's one of the most common questions we hear — usually said with a mix of concern and quiet hope: "My gums have been pulling back. Can they grow back on their own?"
The honest answer? Rarely. But here's the part that actually matters: receding gums don't have to keep getting worse. And catching the problem early — before it becomes painful, before it becomes expensive — is the whole game.
So let's talk about what's really going on when gums recede, why it happens, and what you can realistically do about it.
First, the Biology: Why Gums Don't Just "Bounce Back"
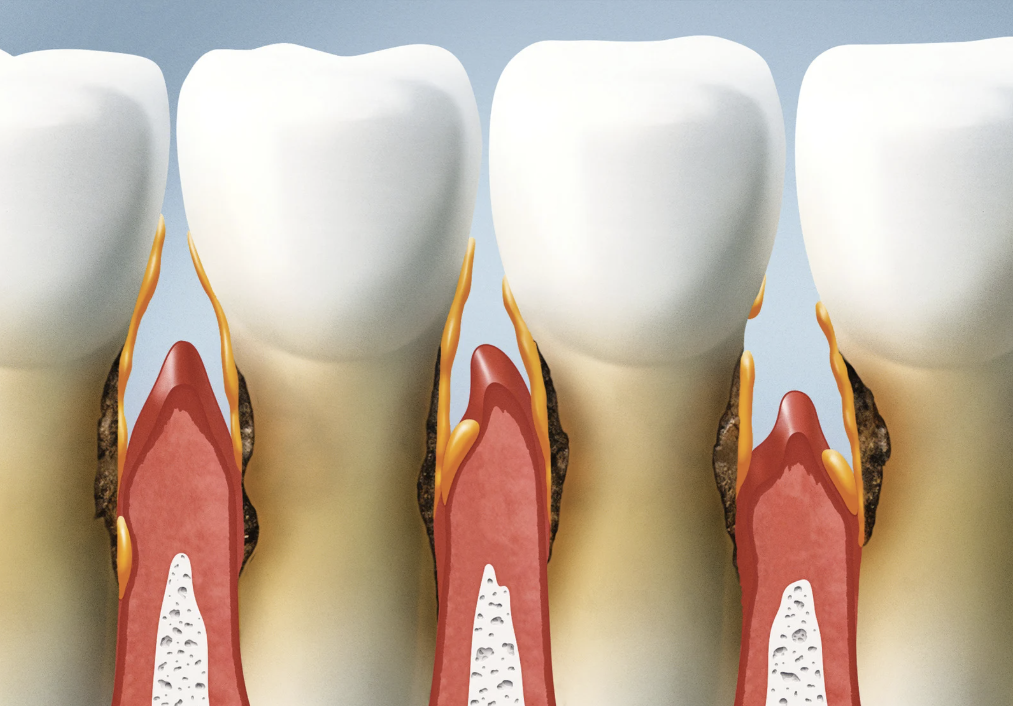
Gum tissue is not like skin. When you cut your finger, the skin regenerates. Gum tissue — particularly the dense, fibrous tissue called keratinized gingiva that forms a protective collar around each tooth — doesn't have that same self-repair ability. Once it recedes beyond a certain point, it doesn't grow back on its own.
That's the clinical reality, and we'd rather tell you plainly than let you discover it after years of waiting for something that isn't coming.
What can happen — and what we focus on — is stopping further recession before it creates bigger problems: tooth sensitivity, root exposure, bone loss, and in advanced cases, loose teeth.
What Actually Causes Gum Recession — It's Not Just "Getting Older"
This is where a lot of people have the wrong picture. Gum recession is commonly dismissed as an unavoidable part of aging, but age is rarely the primary driver. In our practice, the causes we see most often are:
Brushing too hard. This is, genuinely, the number one cause we see. A firm-bristled toothbrush used with heavy pressure — even with the best intentions — mechanically wears away gum tissue over time. It's the dental equivalent of sanding wood: you think you're cleaning, but you're also removing material. A soft-bristled brush and a gentle circular technique makes an enormous difference.
Teeth grinding and clenching (bruxism). The forces generated by nighttime grinding can reach 250 pounds per square inch — far beyond what normal chewing produces. Over time, that sustained pressure on teeth and their surrounding structures causes bone loss and gum recession. Most people who grind their teeth at night have no idea they're doing it until a dentist points it out.
Ill-fitting dental work or misaligned teeth. When a crown, bridge, or filling creates an uneven bite, or when teeth are significantly crowded or misaligned, unequal force distribution leads to localized recession in the overloaded areas. This is one reason orthodontic assessment and proper bite analysis matter even when cosmetics aren't the primary concern.
Chronic inflammation from gum disease. Periodontal disease — the bacterial infection of the gum tissue and bone around teeth — is a major driver of recession. Inflammation breaks down the connective tissue and bone that support the gums. Even low-grade, chronic inflammation that doesn't cause obvious pain does real structural damage over months and years.
Genetics. Some people simply have thinner gum tissue to begin with, making them more susceptible to recession even with excellent oral hygiene. If recession runs in your family, more frequent monitoring is worth it.
Oral piercings and tobacco use. Lip and tongue piercings repeatedly traumatize the gum tissue they contact. Tobacco — in any form — constricts blood flow to the gums, impairs healing, and accelerates bone and tissue loss.
The Sneaky Part: Gum Recession Happens Quietly
Here's what makes gum recession genuinely tricky: it usually doesn't hurt. Not at first.
Gums recede gradually — millimeter by millimeter, over months and years. By the time most patients notice it (often because a tooth starts looking longer, or because they develop sensitivity to cold), meaningful tissue loss has already occurred.
This is exactly why the old advice — "if it doesn't hurt, it's fine" — doesn't apply to periodontal health. The absence of pain is not the absence of a problem.
Regular dental checkups give us the ability to measure gum levels over time and catch changes early, before they cross the threshold where treatment options narrow significantly.
What "Management" Actually Looks Like — Practical and Realistic
If you're dealing with mild to moderate recession, the most important interventions are often the simplest — and they work.
Switch to a soft-bristled brush and change your technique. This alone slows or stops mechanically-driven recession in a significant portion of patients. An electric toothbrush with a pressure sensor is an investment we recommend regularly — it takes the guesswork out of "how hard is too hard."
Address grinding with a night guard. A properly fitted occlusal guard (night guard) distributes bite forces evenly and eliminates the direct pressure on teeth and surrounding tissue during sleep. It's one of the most cost-effective protective devices in dentistry.
Get inflammation under control. Professional cleanings — and in some cases, scaling and root planing (a deeper cleaning that removes bacterial buildup below the gumline) — remove the bacterial load that drives chronic inflammation. When the inflammation goes away, the active recession often stabilizes.
Correct the underlying bite issues. If misalignment or a poorly fitting restoration is contributing to recession in specific areas, addressing that root cause is essential. Treating the gum without fixing what's causing the problem is short-term thinking.
Consider gum grafting for advanced cases. When recession is significant enough that root exposure is causing sensitivity, aesthetics are affected, or the remaining tissue is too thin to be stable, a gum graft — where donor tissue is placed to rebuild the lost coverage — is a predictable, well-established procedure. It doesn't restore tissue that was never there, but it can halt further loss and recover some of what receded.
When Should You Actually Call a Dentist?
We'd say: sooner than you think you need to.
If you notice any of the following, it's worth scheduling an evaluation:
Your teeth look longer than they used to
You're experiencing sensitivity to cold, heat, or sweet foods
Your gums bleed consistently when you brush or floss
You can see the darker root surface of one or more teeth
You've been told you grind your teeth, or you wake up with jaw soreness
None of these are emergencies — but each one is a signal that something is changing, and earlier attention always means more options.
The Part We Say to Every Patient
Gum tissue changes quietly. It doesn't announce itself with pain until the problem is already significant. The patients who fare best long-term aren't the ones who waited until it hurt — they're the ones who came in when something seemed slightly off, got a clear picture of what was happening, and made small adjustments before things progressed.
That's what we're here for. Not to alarm you — to give you accurate information while there's still plenty you can do about it.
Frequently Asked Questions About Receding Gums
Can receding gums grow back on their own?
In most cases, no. Once gum tissue has receded beyond a certain threshold, it does not regenerate on its own. However, with proper management — addressing the underlying cause, improving oral hygiene technique, and controlling inflammation — further recession can be significantly slowed or stopped entirely.
Is gum recession always a sign of gum disease?
Not always. Gum recession can result from aggressive brushing, bruxism, misaligned teeth, or thin gum tissue genetically. That said, gum disease (periodontitis) is one of the most common drivers, which is why a clinical evaluation to determine the actual cause matters — the right treatment depends on the right diagnosis.
Does gum recession hurt?
Usually not — at least not initially. The most common symptom is tooth sensitivity, particularly to cold temperatures, as the root surface becomes exposed. Many patients are unaware of recession until a dentist measures it at a checkup.
How is gum recession treated?
Treatment depends on the cause and severity. Mild cases often respond well to improved brushing technique, professional cleanings, and addressing contributing factors like grinding. More advanced recession may require a gum graft to restore tissue coverage and stability.
How often should I have my gums checked?
For most adults, every six months is standard. If you have a history of gum disease, thin gum tissue, or known risk factors, your dentist may recommend more frequent monitoring — typically every three to four months.
A Note on Caring for Kansas City
We've been a dentist in Kansas City, Kansas since 2003, and over two decades, one thing has stayed constant: the patients who do best are the ones who come in before the problem is obvious. Gum health is quiet — it rarely announces itself until you're already well past the easy fix.
If it's been a while since you've had your gums properly evaluated, or if something has felt a little off lately, this is your nudge. We see patients in English, Spanish, and Korean, and we work hard to make sure the information you leave with is actually useful — not just reassuring.
Give us a call. We'll take a real look and tell you exactly where things stand.
📍 State Avenue Dental Office — Kansas City, KS (KCK) 🗣 English • Korean • Spanish Your implant investment deserves ongoing protection. We're here to help.